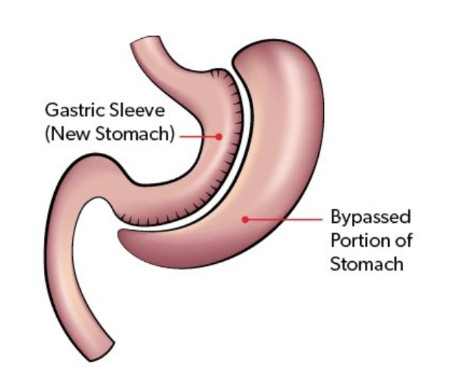
After gastric sleeve surgery, your diet plan may look a bit different depending on your clinic or surgeon, but the core rules don’t change much. Most plans focus on the same basics, the focus on high-protein after gastric sleeve is prevalent in each so it’s easier to follow than it sounds.
- High protein first, at each meal and snack
- Low sugar, avoid sweets, juice, and sugary drinks
- Low fat, choose lean options and limit fried foods
- Hydration is non-negotiable, sip water all day
- Simple structure, small portions, slow eating, and steady progress through food stages
- Clear, written rules matter, so you’re not guessing day to day
- What’s coming next, the exact guidelines I followed after my gastric sleeve, plus two other clinic guides that explain the diet steps well, all in a “Diet Made Simple: High-Protein After Gastric Sleeve” format.

The Perfect Serving will contribute to the weight loss process after surgery, make sure to keep a balance of your daily Macros intake.

SIMPLE STEPS TO A HEALTHY LIFE
- It is important to note that lifestyle and behavioral changes are necessary to be successful with your weight loss journey.
- Eat three meals a day and limit unnecessary- snacking in-between meals. This weight
loss surgery- is a restrictive procedure, which means that the success of weight loss
depends on what you are eating. Unhealthy snacking in-between meals (e.g. pretzels,
crackers, cookies, ere.) or eating frequently may prevent successful weight loss or
cause weight gain due to excess calorie intake. - Eat slowly and chew your food until LIQUID. Failure to do so can cause pain, nausea,
vomiting, heartburn and irritate your new pouch. It is very important to chew very
thoroughly until it is Liquid . Also, remember to cut your food into small pieces
before eating it. Try waiting one minute in-between bites. Allow at least 30 minutes
for a meal. - Avoid concentrated sugar. Keep sugar out of the first 3 ingredients on the food
label. The number of sugar grams on the label includes both added and natural sugars;
therefore, it is important to read the ingredients to find out what type of sugar the food
contains. Aim to keep the “sugars” down to 15 grams or less per serving to help limit
“empty calories” in your diet. Avoid these simple sugars, especially if within the
first 3 ingredients on food labels: sugar, dextrose, high fructose corn syrup, corn
syrup, glucose, sucrose, molasses, and honey Note : Artificial sweeteners such as
NutraSweet/Equal®, saccharin/Sweet’n Low®, and sucralose/Splenda® are
acceptable to use. - Limit high fat foods. Low fat is 3 grams or less per serving on a food label.
Examples of high fat foods: potato chips, fried foods, fast food, bacon, sausage, hot
dogs, bologna, pepperoni, cream soups, Alfredo sauce, donuts, cakes, cookies, and
pastries. - Stop eating when you feel comfortably satisfied. Overeating can cause nausea,
vomiting, and the size of your stomach to stretch. It can take 6-9 months for your new
stomach size to stabilize. - Drink adequate fluids to prevent dehydration. Aim for 64-86 fluids ounces (8 cups
- min) of fluid per day.
- Take small frequent sips of your beverage throughout the day, no gulping!
- Avoid beverages that are carbonated, containing sugar, caffeine and alcohol.
- Choose sugar-free, non-carbonated drinks such as: Crystal light®-, Fruit 20®, Diet Snapple®, Propel Fitness Water, Light Minute Maid® drinks, Diet Ice Tea, etc.
- Limit fat free milk to less than 16 ounces per day, limit 100% real fruit juice to less than 8 ounces per day (try diluting with water).
- TIPS:
- Wean off carbonated and caffeinated beverages before surgery to help prevent withdrawals.
- Choose beverages with 10 calories or less per serving.
- If plain water sits heavy and you are having problems tolerating it add a sugar free flavoring (e.g. True Lemon®, lemon or orange slice, etc.)
- Increase your fluid intake if any of the following signs are present: dark urine, headache, dizziness, lethargy, a white coating on the tongue.
- AVOID eating and drinking at the same time. Avoid drinking with your meal, then
wait at least 30 minutes after a meal to resume drinking. - Choose your food wisely , at each meal protein should be consumed first, then
vegetables and fruits, then “whole” grains. - Exercise!
● Aim for at least 30 minutes every day.
● Exercise helps maintain long-term weight loss.
● Even 5 minutes at a time, as tolerated, is a start, and increase the time and
frequency as tolerated.
● The first four weeks, the primary exercise used should be walking. After four
weeks, try introducing strength exercises.
● Always speak with your doctor if you have never exercised. - Protein . You need to consume at least 60-80 grams of protein per day in the form of
food and/or supplements.


Protein Meal Supplements
There are many brands of supplements available (ready-to-drink or powders). For some examples:
● Look for drinks made with Whey Protein Isolate (this is absorbed well), vs. whey protein concentrate, which has lactose, or milk sugar. Strive for a protein with at least 20 grams of protein per serving. Mix with skim or 1% milk for an additional 8 grams of protein per serving Aim for a product with less than 3 grams of sugar per serving.
Avoid and/or limit protein collagen-based products (incomplete form of protein that is
missing tryptophan, an important building block of protein)
● Examples: Ready to drink – Atkins®, E.A.S. Myoplex Carb Sense®, Zero Carb,
Isopure® Powders – Designer®, Unjury®, Nectar®, Premier protein®
Vitamin and Mineral Supplements. You are required to take supplement for the rest of your life to prevent deficiencies.
● Multivitamin ; Two chewable or liquid multivitamin with minerals per day. Take with
food. Examples: Centrum Chewables®, Flintstone Complete®
● Calcium ; 1500 mg of calcium citrate per day (take one chewable 3 times daily) Maximum of 600 mg at one time for absorption Must contain vitamin D (at least 200 IU) Examples: Twinlab® chewable calcium wafers (2 tab, 3x a day), Citracal® plus D (2 tabs, 3x a day), Solaray Calcium plus D and Mag (2 wafers, 3 times a day).
SAMPLE Table for Taking Your Supplements
Breakfast — Multivitamin (NOT with dairy)
Lunch — 500-600 mgs Calcium
Snack — 500-600 mgs Calcium
Calcium Dinner — 500-600 mgs Calcium
CHECKLIST AFTER YOUR GASTRIC SLEEVE SURGERY
● 60-80 grams of protein a day
● No more than 45 grams sugar a day
● Try to keep fat to under 9 grams a day
● By week 5 you should be having a calorie intake between 800-1200 a day depending on your daily activity
● Eat protein first at all meals
● Eat slowly and chew well
● Meals should take 30-45 minutes
● Avoid snacking on high calorie foods in between meals
● 64-86 oz. of fluid a day (more if your urine is dark or you’re dizzy)
● Beverages less than 10 calories per serving
● Vitamin/mineral supplementation taken for life this may decrease,in amount suggested by your Primary Care Physician based on blood work ups for vitamin
levels. These should be done at the following intervals:
- 3 Months, 6 Months, 9 Months, 1 Year, Once a year after the first year
● Multivitamin (one a day, with food; not with calcium or dairy)
● Calcium citrate 1500-2000 mgs a day…in divided doses (at least 3 times a day) and no more than 600 mgs at one time, and apart from multivitamin and iron
● Exercise Aim for at least 30 minutes on most days of the week…5 minutes at a time, and gradually build up, as tolerated
● Incorporate light weights (about 2 months after surgery, and/or as your surgeon recommends)
● Consider stretching and the importance of a stress management program in your
regimen
The 2nd Clinic is actually more informative than the one information I received when I had my surgery.
Skills for Success
Bariatric surgery is only a tool. You must commit to a healthy lifestyle (diet, exercise, behaviors) to stay
successful forever.

Physical Activity
- Most people need to exercise at least 250 minutes (over 4 hours) each week to maintain weight loss. It takes time to build up to that amount of exercise, but we are here to help you. Even if you don’t reach that level of exercise, any amount of exercise will benefit your body. You can even break your exercise up into smaller amounts of time during the day. It’s about finding what works best for you!
- Here are some ideas for increasing your physical activity before and after surgery.*
- Walk more!
- Walk the dog; go for a walk with a friend, a neighbor, or your children.
- Get up to talk to co-workers instead of sending an email or making a phone call.
- Wear a pedometer to track your steps and challenge yourself to increase steps over time.
- Take a “walking break” at work instead of a coffee break.
- If you take the bus or subway, get off a few stops early and walk.
- Park your car farther away at shopping centers and walk through the parking lot.
- Take the stairs instead of the elevators.
- During foul weather, get exercise by walking in the mall.
- Make exercise a family event. Go for a walk together after dinner or on the weekend.
- Keep exercise clothes in your car to make sure you will go to the gym.
- To decrease impact on your joints, try pool exercises, water aerobics, or a stationary bicycle.*
- Please refrain from swimming until your first appointment after surgery.
- Turn up the music and dance.
- Do yard work, gardening, or household chores that require brisk movement.
- Check out exercise videos online.
- Try chair exercises.
- What does 250 minutes of exercise look like in a week?

What are the benefits of exercise besides weight control?
- Improves mood
- Boosts energy
- Keeps body strong
- Promotes better sleep
- Improves bone health
- Improves heart health
Remember to check with your primary care doctor or surgeon before starting any strenuous exercise.
However, you may start walking right after surgery.
Vitamin and Mineral Supplements:
You will need to take vitamin and mineral supplements for the rest of your life after surgery.
Multivitamin with Minerals:
- Take a ‘complete’ multivitamin(s) daily; dose will vary based on brand of multivitamin.
- Complete multivitamins contain iron, zinc, folic acid, and copper.
- Avoid gummy or soft chew multivitamins – these don’t have all of the right nutrients.
- Separate multivitamin(s) with iron from calcium by at least 2 hours.
- Vitamin B12:
- Take 350-500 micrograms vitamin B12 daily in the form of a tablet or liquid.
- You can take vitamin B12 at any time or with any other supplements.
- You can also get vitamin B12 in a nasal spray or injection.
- Your multivitamin might have enough vitamin B12 in it. This will be listed on your shopping guide.
- Calcium Citrate with Vitamin D:
- Take 1200-1500 mg of calcium citrate daily split into 2-3 doses.
- Your body can only absorb 600 mg of calcium at one time.
- Separate calcium doses by at least 4 hours.
- Separate calcium from multivitamins by at least 2 hours.
- You can also meet your daily calcium needs from food and supplements. Talk to your dietitian.
- Other Supplements:
- Some patients may need extra vitamins and minerals, such as iron, vitamin D, or B vitamins. We will check your vitamin and mineral levels regularly through lab tests and discuss extra supplements as needed.
Meal Plan
Starts: 40 days after your surgery date
Last for: Forever, but your meal plan will change over time.
What to Do: Keep sipping fluids. Use the meal plan below as guidance for a balanced diet. Keep taking
vitamin and mineral supplements.
Fluid Goal: 48-64 ounces
Protein Goal: 60-70 grams/day
Meal Plan
- 8 cups of fluid
- 8 protein servings
- 2 vegetable servings
- 2 fruit servings
- 1 dairy serving
- 2 fat servings
- 3 starch servings
Use the meal plan for guidance. In the early months after surgery, you won’t have room for all of the foods in the meal plan. Focus on foods from the protein, vegetable, and fruit groups first.


Sample Meal Plans
These are examples to show you how the amount you can eat will change over time. Each person can choose their own foods based on their preferences and their tolerance.
Just starting Stage 4 – about 6 weeks after surgery
- 8 cups of fluid
- 8 protein servings
- 2 vegetable servings
- 2 fruit servings
- 1 dairy serving
- 2 fat servings
- 3 starch servings

Feeling comfortable with Stage 4 – about 8 months post-op
- 8 cups of fluid
- 8 protein servings
- 2 vegetable servings
- 2 fruit servings
- 1 dairy serving
- 2 fat servings
- 3 starch servings


Long-term Stage 4 – About 2 years post-op
- 8 cups of fluid
- 9 protein servings
- 2 vegetable servings
- 2 fruit servings
- 1 dairy serving
- 2 fat servings
- 3 starch servings


Protein Foods

Non-Starchy Vegetables


Fruits

Dairy

Fat

Starches

The 3rd Clinic is very informative, probably more than the information I received when I had my surgery.

Preparation Goal: Establish a Consistent Meal Routine
After bariatric surgery, you must eat regular meals and snacks to make sure you are meeting your
nutrition requirements. An erratic eating schedule, long gaps between meals, or skipping meals
can result in sub-optimal weight loss, nutrient deficiencies, malnutrition or, ultimately, regaining
your weight.
You need a consistent meal routine before your surgery. This is an essential part in preparing for
post-bariatric life.
A consistent meal routine is:
- Not skipping meals
- Eating 3 well-balanced meals a day
- Eating your first meal within 90 minutes of waking
Not going longer than 4 to 6 hours between meals - Adding a small, healthy snack between meals, if it is more than 5 hours until your next meal.

Preparation Goal: Eat Well-Balanced Meals
A well-balanced meal includes foods from the different food groups and provides a variety of
nutrients. After bariatric surgery, you will need to consume balanced meals to make sure you are
getting the vitamins and minerals you need to stay healthy.
The “Healthy Plate” is a visual diagram that can help you eat well-balanced meals. Eating
according to the Healthy Plate can help you:
- Eat appropriate serving sizes to manage your weight
- Optimize your nutrition
- Increase your sense of fullness
- Avoid eating too much of any one food group
- Include a source of lean protein at each meal, which is essential after surgery


- Protein: Choose lean meats, poultry, fish, beans, and low-fat dairy
- Grain/Starch: Look for whole grain items.
- Vegetables/Fruits: Choose a variety of colors.



Preparation Goal: Plan Your Meals
Planning meals in advance will help you stay on track with your meal routine and overall weight
management goals. It also helps you manage your time better, makes preparing meals easier, and
prevents you from making poor food choices when you are busy.


Preparation Goal: Read Nutrition Facts Labels
Reading and understanding food labels is important when choosing what to buy at the grocery
store. It helps to make sure you are meeting your nutritional needs and making healthy food choices.

How do I read an ingredient list?
In addition to checking the Nutrition Facts label, get in the habit of reading the Ingredient List. This list tells you what the food is made of, which is important if you have a food allergy or intolerance. Ingredients are listed in order by weight. The first ingredient is highest in weight.

How do I check for sugars in packaged foods without a Nutrition Facts label?
Sugar: Look at the ingredient list and find ‘sugar’. If sugar is one of the first 3 ingredients on the list,
do not eat that food, as they are too high in sugar and may cause dumping syndrome.






Preparation Goal: Identify and Manage Emotional Eating
What is emotional eating?
Humans need to eat so our bodies and brains function properly, but sometimes we eat for reasons
other than biological hunger. Emotional eating is a term that refers to eating when we feel certain
emotions, including anger, stress, boredom, loneliness, or happiness.
When eating is your primary emotional response or coping mechanism, the unintended effect is
weight gain. You also do not examine the root cause or the emotion thoroughly and deal with it in a
healthy manner.
Am I an emotional eater?
- Do you eat more when you’re feeling stressed?
- Do you eat when you’re not hungry or when you’re full?
- Do you eat to feel better (such as when you’re sad, mad, bored, anxious)?
- Do you reward yourself with food?
- Do you regularly eat until you’ve stuffed yourself?
- Does food make you feel safe? Do you feel like food is a friend?
- Do you feel powerless or out of control around food?
- Do you have a habit of eating at a certain time of day (for example, you snack at 9:00 p.m. daily)?

What are the common causes of emotional eating?

- Stress: When stress is chronic, it leads to high levels of the stress hormone cortisol. Cortisol triggers cravings for salty, sweet, and high-fat foods. The more uncontrolled stress you have in your life, the more likely you are to turn to food for emotional relief.
- Hiding emotions: Eating can be a way to temporarily silence uncomfortable emotions, such as
anger, fear, sadness, anxiety, loneliness, resentment, and shame. While you consume food, you
do not feel the full effects of your emotions, resulting in a temporary sense of relief. - Childhood habits: Think back to your childhood memories of food. Did your parents reward
good behaviour with ice cream, or take you out for pizza when you got a good report card?
Was food scarce, restricted, or used as a punishment for you? These emotionally-based childhood
eating habits often affect your relationship with food in adulthood. - Boredom or feelings of loneliness: Eating food or snacking is often used to pass time.
An example can be opening the fridge and eating something, even though you’re not actually
hungry. Another example is having the urge to snack on candy despite having just had a meal.
These would be considered boredom eating. Consuming food can also be a way to mask
feelings of loneliness. - Social influences: Getting together with other people for a meal is a great way to relieve stress,
but it can also lead to overeating. It’s easy to overindulge simply because the food is there or
because everyone else is eating. Your family or circle of friends may encourage you to overeat,
and it’s easier to go along with the group.
NOTE: If you rely on food to cope with your emotions, you are at risk of developing
unhealthy coping mechanisms after surgery. There is an increased risk of substance
abuse after bariatric surgery, called transfer of addiction.
How can I manage emotional eating cravings?
Managing emotional eating cravings can be difficult, especially if you have tried to resist them in the
past without success. Remember that these cravings are trying to meet an underlying emotional
need. If you do not find a way to meet that need in a healthy way, you will always rely on food or
other unhealthy/dangerous addictions and habits to cope.
The following are some healthier alternatives to managing emotional eating cravings.
- Keep an Emotional Eating Diary: One effective method is to track your eating habits with
a food and mood log (see example below). When you review your log, you can have a better
understanding of what triggers you to eat.
Be mindful to keep track of:
» What you ate (or wanted to eat)
» What happened to upset you
» How you felt before you ate
» What you felt as you were eating, and
» How you felt afterward.
Over time, you will see a pattern emerge. Once you identify your emotional eating triggers (or
food triggers), the next step is to identify healthier outlets.

- Get Enough Sleep: Lack of sleep has a direct link to stress, overeating, and weight gain. When you do not get the sleep you need, your hunger hormone levels rise, stimulating your appetite. As well as making it harder to fight food cravings, feeling tired can also increase your stress levels, leading to more emotional eating. To control your appetite and reduce food cravings, try to get plenty of rest; about 8 hours of quality sleep every night.
- Practice Self-Care: You can do many things to help to nurture yourself and meet your emotional needs. Make sure that you are giving yourself a mental health break at least once a week or, ideally, 1 to 2 times a day.
Self-Care Ideas
- Play with companion animals
- Knit, crochet, sew, etc.
- Colour adult colouring books
- Read
- Take up photography
- Play board games, crosswords
- Listen to music
- Do some gardening
- Go for a walk
- Talk to a loved one
- Volunteer in the community
- Do puzzles
- Connect with mental health supports
Use a Hunger Scale: Using a hunger scale can help you identify the type of hunger you are
experiencing. This will help you make sure you are eating due to physical hunger and not
because of emotional hunger or cravings (also known as mouth hunger). Eating regularly will
help prevent you from feeling really hungry or really full.


Practice Mindful Eating: Often, our mind wanders from what we are doing in the moment, leading us to
go about our day mindlessly; including when we eat. Mindful eating means paying attention to what you
are eating, when you’re eating it, before it’s all gone! It also means learning to listen to your body and
knowing when you are hungry and when you are full. Reconnecting with and listening to your body and
feelings of fullness and hunger are the first steps to addressing emotional eating tendencies.
Preparation Goal: Get Active!

Studies have shown that exercising regularly before having bariatric surgery can actually reduce the risk of surgical complications and enhance recovery. The American Society for Metabolic and Bariatric
Surgery (ASMBS) recommends that a patient undergoing bariatric surgery engage in mild or moderate exercise for 20 minutes a day, 3 to 4 times a week before surgery. Mild to moderate exercise includes cardio or strength-based exercises that allows you to still talk regularly while exercising, without pausing to gasp for breath. Choose exercises that you enjoy doing. This is the best way to create healthy, long-lasting habits.
NOTE: If you do not regularly engage in physical activity, please have your doctor or specialist medically clear you first before you begin to exercise.
Preparation Goal: Plan for Pregnancy Prevention
Avoid pregnancy for the first 2 years after surgery. Pregnancy during this time could cause complications and nutritional deficiencies for you and your baby and may result in birth defects.
NOTE: Rapid weight loss increases fertility so even if you had problems getting pregnant before surgery, you should still be careful to prevent pregnancy. We do not recommend using oral birth control pills for contraception as they will not be fully absorbed after surgery. Please speak to your family doctor about
non-oral birth control options
Introduction to Solid Foods







Choosing a Protein Supplement

Taking Vitamin and Mineral Supplements



Strength Training

Diet Recommendations at 6 Months Post-Op and Beyond
Paying attention to portion size is important when it comes to long-term weight loss success or
weight maintenance. You may begin to feel that you do not have as much restriction, or are able to
eat more. However, it is even more important to be intentional about your portion sizes.


Body Image and Body Acceptance
After bariatric surgery, your body may feel unfamiliar. Your body image (your subjective mental
picture of yourself) may have also changed, either in a positive or negative way. You may also have
concerns related to excess skin.
Body image is linked closely to self-esteem and can significantly change how you feel about yourself.
As a result, it is important to work on cultivating a healthy relationship with your body or body image
after surgery.
If you are struggling with your body image, you may find it helpful to focus on body acceptance
instead. Body acceptance means developing a non-judgmental relationship with your thoughts,
emotions, and physical self. It is acknowledging that there may be some parts of yourself which you
don’t necessarily love, but not allowing this to determine your self-worth.
What can I do to build a healthy body image?
- Pay attention to the words you use when talking about yourself to others or when engaging in
self-talk. - Work on being more mindful of your thoughts and words. Try to re-frame your comments about
your body in a positive way. - Do positive things for yourself on a regular basis (for example, get a massage or work on a new
skill, hobby). - Remind people in your close circle to not comment on changes to your body and to avoid
commenting on body size in general. - “Block” or “unfollow” accounts on social media that make you feel insecure or judged. Find
accounts that promote body positivity and acceptance of bodies in all shapes and sizes. - Practice “Body Acceptance Statements” with yourself:
» “I am grateful for what my body does for me every day.”
» “I am so much more than what my body looks like.”
» “Bodies come in different shapes and sizes, and this does not change their worth.”
» “There is more to life than worrying about my weight. I’m ready to experience it.”
» “My existence makes the world a better place.”
» “My appearance and body size will change… that’s normal.”
» “My healing process is unique to me, and I honor each milestone.”
If you find that a negative body image is disrupting your everyday activities, speak to
your primary care provider and call the Bariatric clinic to book an appointment with
one of our social workers.
What is high intensity exercises?
You can now begin to do high intensity cardio exercises, if you are medically cleared to do so.
Continue to aim for 150 to 300 minutes of cardio-based activity a week (that is, 30 to 60 minutes a
day), as well as 2 to 3 days of strength training.
Find exercises that you enjoy! This can include group classes or online videos. If you need help
developing an exercise routine, call the Bariatric clinic to book an appointment with the kinesiologist.
During high intensity exercises:
- You have a significantly elevated heart rate
- Your body temperature increases quickly
- You need to pause for breath between words
Tip! Have a meal 1 hour before exercise, or a small snack 30 minutes before exercising
to fuel you for exercise without making you feel overly full or uncomfortable. Exercising
on an empty stomach may cause low blood sugars, dizziness, and may cause you to
feel tired faster. Make sure to have a small portion of carbohydrates in your meals and
snacks for energy
Defining Success After Bariatric Surgery
Bariatric surgery is a tool to help you live at, and maintain, your “best” weight. This may differ from
your expected “ideal” weight. The goal after the first year is to maintain this “best” weight in the long-term. Your best weight is unique to you, and allows you to live your healthiest life while still having a fulfilling and satisfying life (that is, not over-restricting yourself).
Addressing Weight Regain
It is possible to experience some weight regain beyond the first year. Normal weight regain is about
5% to 8% regain of the weight you lost (that is, if you lost 100 lb, you may regain 5 to 8 lb).
Weight regain beyond this is typically considered behavioral weight regain and is caused by
lifestyle and diet habits, such as:
- Unhealthy eating patterns, such as grazing, nibbling, skipping meals, mindless eating
- Eating beyond the point of fullness
- Not eating enough protein or fibre at meals (balanced meals)
- Improving or losing dumping syndrome symptoms
- Choosing high calorie food and beverages
- Increasing portion sizes
- Eating and drinking at the same time
- Emotional eating
- Lacking self-monitoring and self-monitoring tools (journaling, weighing, and measuring foods)
- Lacking sleep and having chronic stress
- Lacking physical activity
- Taking certain medicines.
If you notice weight regain, the first step to getting back on track is addressing these habits.
Meal Planning Skills to Manage Your Weight for Life
Successful long-term weight loss requires permanent lifestyle changes. If you go back to your old
eating habits, you will start to regain your weight. It may start out as only a few pounds per year, but
that can add up to a significant weight gain if the pattern continues.
The most important thing you need to do is make sure that your environment is set up for success.
Think back to the tools you used when you first had surgery. If you find that you are starting to gain
weight, use your measuring cups and food scales, make your meal plans and grocery lists, and start
keeping a food journal again.
Sticking with your meal routine, eating balanced meals, and making healthy food choices is very
difficult if you don’t have healthy food ingredients on hand. Meal planning, even if only for 1 to
2 days in advance, is a key skill to help you maintain your weight loss


Avoiding Over-Restriction
Real life includes the occasional chocolate, ice cream, pizza, or fries. If you try to cut out all foods
you have labelled as “bad”, then over time those feelings of being restricted or deprived can lead to
cravings and possibly binging on a “forbidden” food.
Instead of labelling food as “bad” or “off limits”, work them into your meal plan and plan for the
occasional treat. However, before you eat one of these foods, ask yourself the following:
- Is it worth the calories?
- What is the smallest amount of this food I can have and still be happy?
- What is the smallest amount of this food I can have and still work towards my weight loss goals?
- Why am I craving this food? Did I skip meals or snacks? Did I eat enough at my meals?
Did I balance my plate? Am I eating in response to a cue or trigger?
Eating Out

Eating away from home may be an important part of your social life, but it is challenging to maintain your weight when you eat out too often. Even sit-down restaurants can be hazardous to healthy eating as the choices are often high in calories, fat, and sodium!
Make sure your meal fits into your meal plan. It is best if you can limit eating away from home to one or fewer times per week or ideally month.

Checklist for Staying on Track Beyond the First Year

Dumping Syndrome
You may experience dumping syndrome after consuming foods or drinks that are high in fat or sugar,
or eating and drinking at the same time. Dumping syndrome happens when these foods move
too quickly through your stomach pouch and into the small intestine. Food is “dumped” into the
small intestine before it can be broken down in the stomach.
Signs and symptoms of dumping syndrome include:
- Sweating
- Dizziness
- Weakness
- Nausea
- Cramping
- Vomiting
- Diarrhea
- Loose stools
- Heart palpitations

Gas and Bloating
Gas and bloating is common, especially during the first few weeks after surgery. It could also be a
sign of lactose intolerance.
Gas or bloating can be due to:
- Taking antibiotics or other medicines
- Drinking carbonated beverages or eating gassy foods
- Eating too quickly, drinking through a straw, chewing gum, or other actions that cause you to
swallow air - Conditions, such as lactose intolerance, where the intestines are not able to digest and absorb
certain foods. You can develop lactose intolerance after having bariatric surgery - A gastrointestinal infection, blockage, or disease
- Irritable bowel syndrome (IBS)
- Constipation, since the longer food waste remains in your colon, the more time it has to ferment